The Bridge Between Sweets and Cavities: Your Oral Microbiome
Growing up we have all heard the warning: “If you eat too many sweets, you’ll get cavities.” But, that’s just a part of the “hole” truth. By that logic, everyone who loves desserts would constantly get tooth decay. So, what’s actually going on?
Our teeth are coated with a thin, sticky film called dental plaque. This plaque consists of a community of bacteria that forms a protective, sticky layer made up of polysaccharides.
Even after brushing and flossing, this layer starts to reform again within minutes. That’s because our mouth is home to hundreds of microorganisms which are constantly attaching themselves to surfaces and rebuilding their communities. In many ways, plaque is an ecosystem of its own. And just like any other ecosystem, it requires balance.
Factors affecting the oral microbial composition
No two people have exactly the same microbial composition. While many of us share similar types of bacteria, the proportions of those bacteria can vary from person to person. A person’s oral microbiome is shaped by genetics, diet, saliva flow, hygiene habits, and even medications.
Role of diet and oral microbiome caries progression
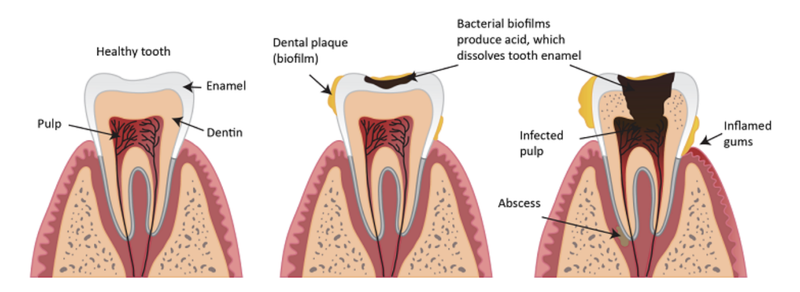
Enamel is the hard, outer most protective layer of the teeth. It is composed of mineral crystals made up of calcium and phosphate. When enamel is exposed to the acid repeatedly, these minerals slowly dissolve in a process known as demineralization, ultimately leading to cavities.
There are several factors that might lead to the formation of cavities, including the diet, oral microbiome and the host physiology.
When we consume sugar or refined carbohydrates, the bacterial community within the plaque uses the sugar molecules as a source of energy, by breaking down the sugars into acids. Research suggests that within minutes of consuming sugar, bacteria in plaque begin producing acids that lower the pH in the mouth. This acidic phase is strongest during the first 30 minutes and may take a couple of hours to return to normal. If the sugar is consumed again , then there is no time for the saliva and enzymes to reset the pH of the oral cavity, and this might affect the teeth's health.
For example, imagine someone eats their favorite sweet during lunch. The mouth becomes acidic for a short period because bacteria in plaque break down the sugars and produce acid as a by-product. If no more sugar is consumed, saliva can gradually neutralize the acid , protecting the enamel against further damage. However, if the same person eats a sweet at lunch, then has a sugary drink within the next hour, and later eats sugary snacks again, the mouth may not have enough time to recover. These repeated acid attacks keep the teeth in an acidic environment for longer, increasing the risk of cavities.
Succession of oral microbes responsible for caries
Regular consumption of sugary drinks or sweets, makes surplus nutrient availability for the oral bacterial community to thrive. As the sugar molecules are being metabolised by oral microbes, the acids accumulate in the oral cavity. This acidic environment leads to the shift in the oral microbial community, favouring the growth of the microbes that can tolerate the acidic conditions. Bacterial species, such as Streptococcus mutans and Lactobacillus species, are able to survive and continue growing even when the pH drops. They are both acid-tolerant and acid-producing, meaning they can withstand low-pH environments and continue metabolizing sugars in ways that contribute to enamel damage and increase the risk of tooth decay.
Another factor that may influence the oral environment is gastrointestinal health. In conditions such as gastroesophageal reflux disease, stomach acid can reach the oral cavity and lower the pH around the teeth. These acidic episodes may contribute to enamel erosion and may potentially influence the microbial balance in the oral cavity.
Tips for Better Oral Health
Reduce the frequency of sugar intake : It’s not just how much sugar you eat, but how often. Giving your mouth time to recover between meals allows saliva to neutralize acids and repair early damage.
Avoid constant sipping and snacking: Slowly drinking sweetened beverages or grazing throughout the day keeps the mouth in an acidic state for longer periods.
Brush before bed — every night: Saliva flow decreases while you sleep. That means bacteria have a longer window to produce acid if plaque isn’t removed.
Stay hydrated: Saliva is one of your body’s strongest natural defenses. Drinking enough water helps maintain adequate saliva flow.
Use fluoride toothpaste: Fluoride strengthens enamel and makes it more resistant to acid attacks.
Don’t aim for sterility — aim for balance: The goal isn’t to eliminate all bacteria. It’s to prevent acid-producing species from dominating the ecosystem.
Conclusion
In conclusion, a healthy mouth isn’t supposed to be microbe free; it needs to be balanced. Cavities don’t begin the moment you eat a piece of candy. They begin when repeated environmental changes shift the balance of the oral microbiome. Sugar fuels the process, but bacteria drive the damage. And once we understand that, prevention becomes less about fear and more about maintaining balance. So next time you are snacking on a sugary treat, ask yourself how many times you have already had one.
-Jayanthi S
Also Read: Digestive distress? The Secret Fix Might Start From Your Mouth!
References
Alavi, G., Alavi, A., Saberfiroozi, M., Sarbazi, A., Motamedi, M., & Hamedani, S.h (2014). Dental Erosion in Patients with Gastroesophageal Reflux Disease (GERD) in a Sample of Patients Referred to the Motahari Clinic, Shiraz, Iran. Journal of dentistry (Shiraz, Iran), 15(1), 33–38.
Featherstone, J. D. B. (2000). The science and practice of caries prevention. Journal of the American Dental Association, 131(7), 887–899. https://doi.org/10.14219/jada.archive.2000.0307
Lv, C., Wang, Z., Li, Z., Shi, X., Xiao, M., & Xu, Y. (2025). Formation, architecture, and persistence of oral biofilms: recent scientific discoveries and new strategies for their regulation. Frontiers in microbiology, 16, 1602962. https://doi.org/10.3389/fmicb.2025.1602962
Marsh, P. D. (1994). Microbial ecology of dental plaque and its significance in health and disease. Advances in Dental Research, 8(2), 263–271. https://doi.org/10.1177/08959374940080022001
Marsh, P. D. (2003). Are dental diseases examples of ecological catastrophes? Microbiology, 149(2), 279–294. https://doi.org/10.1099/mic.0.26082-0
Spatafora, G., Li, Y., He, X., Cowan, A., & Tanner, A. C. R. (2024). The Evolving Microbiome of Dental Caries. Microorganisms, 12(1), 121. https://doi.org/10.3390/microorganisms12010121
Stephan, R. M. (1940). Changes in hydrogen-ion concentration on tooth surfaces and in carious lesions. Journal of the American Dental Association, 27(5), 718–723.
Takahashi N, Nyvad B. The Role of Bacteria in the Caries Process: Ecological Perspectives: Ecological Perspectives. Journal of Dental Research. 2010;90(3):294-303. doi:10.1177/0022034510379602
Tan, X., Wang, Y., & Gong, T. (2023). The interplay between oral microbiota, gut microbiota and systematic diseases. Journal of oral microbiology, 15(1), 2213112. https://doi.org/10.1080/20002297.2023.2213112
Zhang, J. S., Chu, C. H., & Yu, O. Y. (2022). Oral Microbiome and Dental Caries Development. Dentistry journal, 10(10), 184. https://doi.org/10.3390/dj10100184